What is Glaucoma?
Elevated eye pressure is a major risk factor and the cause of glaucoma. The high pressure in the eyes typically damages the eye’s optic nerve in one or both eyes. It commonly occurs in people over the age of 40 and results in vision loss and blindness due to glaucoma. Our Glaucoma Specialist in Kharghar explains more about this dreadful eye condition.
Changes to vision caused by glaucomatous damage are usually quite slow and gradual
this makes the changes difficult to notice in their early stages. Patients diagnosed with glaucoma eventually developed tunnel vision. The space in front of the eye is known
as the anterior chamber a clear fluid called aqueous humor flows continuously in and out of the anterior chamber and nourishes nearby tissues.
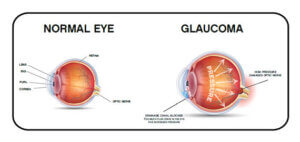

Types of Glaucoma
There are two main kinds of glaucoma:
1. Open-angle glaucoma:
2. Angle-closure glaucoma.
1. Open-angle glaucoma:
Normally, this fluid leaves the anterior chamber at the open angle where the cornea and iris meet through a spongy meshwork. A healthy eye usually balances the rate of fluid production and the rate of fluid drainage out of the eye through this meshwork to
maintain normal pressure in the eye. However, in open-angle glaucoma which is the most common form of glaucoma even though the drainage angle is open, the fluid passes too slowly through the meshwork drain and as fluid builds up in the eye the pressure inside the eye rises to a level that may damage the optic nerve resulting in vision loss.
2. Angle-closure glaucoma.
In contrast, angle-closure glaucoma is caused by complete and total blockage of drainage canals resulting in a sudden and extreme rise in eye pressure, and this demands immediate medical attention. Without treatment, people with glaucoma will slowly lose their peripheral or side vision. Glaucoma detection requires a comprehensive dilated eye exam and includes the following:
• Tonometry measures the fluid pressure in the eye. This is an examination of the optic nerve head and retinal nerve fiber layer.
• Perimetry provides a visual map and quantified evolution of your vision gonioscopy and assesses the anatomical angle formed between the cornea and the iris.
• Pachymetry is a measurement of cornea Thickness.
• OCT – an optical coherence tomography or oct is a detailed eye scanning system.
Are You at Risk of Getting Glaucoma?
Risk factors include:
1. Being over 40 years of age
2. Family history of eye injury or post-surgical complications
3. Being nearsightedness or myopia
4. Long-term steroid use
5. Heart disease and high blood pressure
6. Diabetes
7. Hypothyroidism
What is the Treatment Available for Glaucoma?
Treatments include:
1. Medicines
2. Laser
3. Conventional surgery
4. Or a combination of any of these
Medicines in the form of eye drops are the most common early treatment for glaucoma.
Glaucoma medications are only effective if used daily as prescribed.
Laser Trabeculoplasty:
Laser Trabeculoplasty a high-intensity beam of light is used to make several evenly spaced burns that stretch the drainage holes in the meshwork to help fluid drain out of the eye. There is no reversal of the site already damaged by glaucoma.
Early Detection of Glaucoma:
Regular eye examinations and treatment can prevent blindness from glaucoma. To know more about glaucoma consult our Glaucoma specialist in Kharghar today.
You can book an appointment at Utsav Eye Clinic if you have any symptoms of glaucoma.
More
The National Eye Donation Fortnight is observed every year from 25thAugust to 8th September. The aim of the campaign is to create mass public awareness about the importance of eye donation and to motivate people to pledge their eyes for donation after death.
What is Eye Donation?
Eye donation is an act of donating one’s eyes after his/her death. People who are visually impaired due to corneal disease can be benefited. It is an act of charity, purely for the benefit of the society and is totally voluntary. It is done after death. So eye-donation should be encouraged as one of the best means of social service. To enable another person obtain vision is one of the best forms of charity. Even after death the donor lives in the eyes of recipient. Eyes from a dead person can enable two blind people to acquire vision.
What is the use of eyes received?
The eyes, which are received through such magnanimous gestures, are of great benefit to the society. The front, clear and transparent tissue of the eye called as cornea can be used to restore vision to corneal blind person. The other portions of the eye are also used for research and training purposes to develop cures for some of the common eye diseases.
What is Corneal Blindness?
The Cornea is the clear tissue covering the front of the eye. It is a focusing element of the eye. The Vision is dramatically reduced or lost if the cornea becomes cloudy. This loss of the vision is referred as corneal blindness.
Is there a cure for corneal blindness?
Yes. Removing the damaged cornea and replacing it with a healthy cornea by surgery can cure corneal blindness. Till date the treatment of the corneally blind people is corneal grafting. Artificial corneas have not yet been developed and hence the only source for cornea is from our fellow human beings.
How can one donate eyes?
The eyes of a dead person can be used only if they are taken out within 6 hrs of death. When a person who has given consent for the donation of one’s eyes dies, the eye should be kept wet by sprinkling water on them. Otherwise pieces of cotton wool soaked in water should be placed on both the eyes so that the cornea does not become dry till the eye-surgeon arrives. After the removal of the eyes the eyelids will be stitched together and there will be no visible sign of the eyes having been removed. The entire process is completed within 10-15 mins, therefore if one pledged to donate his eyes after death, it is the duty of his relatives to inform to the nearest eye bank after his death.
How to register: http://ebai.org/donator-registration/
After the removal of eyes, would there be any complications or disfigurement?
There are two methods adopted for removal of eyes. Some eye banks would remove the whole eyeball. In such a case there may be temporary bleeding. The team is well trained to take care of such eventualities. There would be no disfigurement. The eye bank team, after the removal of eyes would properly close the eyes so that there is no disfigurement. The second method is the removal of only the clear transparent tissue. Here also a plastic shield is placed in place of the tissue and no difference can be noticed.
Is eye donation against religious principles or traditions?
All religions endorse eye donation. There are numerous examples in our traditions and scriptures, which endorse eye and organ donation. A part of the body would be consumed by flames and reduced to ashes or which is buried and allowed to decay and disintegrate & cannot be put to a better use than restoring vision to the needy.
Am I too old/young to be an eye donor?
No. There is generally a use for eyes of any age.
Can the eyes of the individuals having diabetes, hypertension be donated?
Yes. People with systemic diseases can also donate eyes.
Who cannot donate their eyes?
Patients suffering from Rabies, Tetanus, Aids, Jaundice, Cancer, Gangrene, Brain Tumor, Food Poisoning, Septicemia & a person who has died due to drowning etc. cannot donate their eyes.
For more information, kindly visit
http://www.v2020eresource.org/content/files/EYEBANK_FAQ/eyebankfaq.htm
https://www.nhp.gov.in/national-eye-donation-fortnight-2016_pg
More
Headaches behind the eyes are common, and they may result from underlying health issues ranging from eye strain to migraine.
Eyestrain
Focusing and refocusing on a screen for long periods can cause eye strain, which can also result from problems with vision.
Fatigue from eye strain can cause pain behind one or both eyes. A person may also experience pain in their eyes or blurry vision.
Causes
Some underlying health issues that cause eye strain include:
optic neuritis, which is inflammation of the optic nerve.
scleritis, which is severe inflammation of the white part of the eye
glaucoma, a disease that affects the optic nerve
Graves’ disease, an autoimmune disorder
Staring at a computer, TV, or phone screen for long periods can also cause eye strain.
Migraine
In addition to a migraine headache, a person may experience:
- eye pain
- dizziness
- weakness
- nausea
- sensitivity to light and sound
- mood changes
- vomiting
- impaired vision
Causes
While doctors are unsure what, precisely, causes migraine, they recognize several common triggers. These are not the same for everyone.
Migraine triggers may be:
emotional, such as stress or anxiety
dietary, such as chocolate or alcohol
physicals, such as a lack of sleep or poor posture
hormonal, such as menstruation
environmental, such as strong smells, smoke, or flickering lights
medication-related, involving sleeping pills or hormone therapies, for example
And More Problems Like
Sinusitis
Cluster headaches
Tension headaches
Treatment
Avoiding the various factors below can often help relieve or prevent pain behind the eyes:
- loud noises
- strong perfume and other odors
- infections
- alcohol use
- hunger
- stress
- changes in hormones
- fatigue
- bright lights
- a lack of sleep
Over-the-counter pain medication can often relieve mild or moderate headaches, but when the pain is severe, prescription medication may be necessary.
Utsav Eye Clinic
Dr. Anand Kumar
Kharghar Navi Mumbai
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
Eye Problems Due to Prolong Use of Mobiles, Tablets, Laptops, Desktops & Televisions, etc.
Since technology is such an integral part of our life, most of us spend many hours staring at screens today, whether they are computers, televisions, or our smartphones. This can cause severe strain on our eyes and vision, and lead to many symptoms like headaches, watery eyes, gritty eyes, sore and red eyes, along with neck and back strain. Computer Vision Syndrome refers to such a state where our eyes start getting these sorts of symptoms over a period.
Working adults aren’t the only ones who are dealing with Computer Vision Syndrome. Even children, who use tablets and gaming devices have seen an increase in the symptoms.
Causes of a Computer Vision Syndrome
There are four main reasons for this syndrome:
Staring at a bright, lit screen means your rate of blinking decreases. This causes dry eyes which causes symptoms like grittiness, foreign body sensation, “sand in eyes” feeling, redness and soreness of eyes.
Prolonged staring for near vision results in convergence spasm of the small eye muscles since the eyes are not geared for prolonged near work. This causes headaches, and also sometimes, inability to focus.
Neck and back staring are the result of improper posture and improper positioning of the computer screen or desk, and also using inappropriate chairs. Reading in bed from screen devices also causes significant problems.
You’re more likely prone to this syndrome if you all ready have any preexisting dryness of the eyes, or if you are not wearing the correct power of glasses.
Treatment of Computer Vision Syndrome
Computer Vision Syndrome is a lifestyle disease, and therefore, its prevention is better than its cure. Minor lifestyle modifications can ensure that you enjoy all your screen devices without any hassles.
The changes that you can easily make in your life to avoid the syndrome include:
Limit screen time: Make sure you are aware of the amount of time you spend on-screen devices and try to decrease your dependence on smartphones.
Ensure proper posture: Make sure your keyboard is positioned to support your wrists, and your computer screen is positioned so that you can look down on the monitor. Optimally, the computer screen should be 15 to 20 degrees below eye level (about 4 or 5 inches) as measured from the center of the screen and 20 to 28 inches from the eyes. Do not read off-screen devices in bed, or in a semi-reclining
Take appropriate breaks: Do not stare at a screen without taking breaks. Remember to follow the 20-20-20 rule; take a 20-second break to view something 20 feet away every 20 minutes.
Think and Blink: Remember to blink since blinking helps redistribute the tear film, and prevents dryness of the eyes.
Proper light: Ensure that there is proper ambient lighting and do not work in the dark. Also, avoid glare from screens by adjusting its brightness, and ensuring the adequate position of ambient lights.
Wear spectacles: Make sure your vision problems are treated, and your eyeglasses prescription is up to date. Limit the use of contact lenses since they aggravate dryness and strain.
Use teardrops: Use over the counter, preservative-free lubricating eye drops to soothe your eyes. Do not use honey, rosewater or other home remedies. Do not self-medicate, or use steroid drops unless prescribed by an ophthalmologist.
See your eye doctor: In case your symptoms persist, please make sure you seek a comprehensive eye examination with your eye doctor since these symptoms can sometimes signify other diseases including undiagnosed refractive errors.
Our Team
Dr. Anand Kumar
Utsav Eye Clinic
Kharghar Navi Mumbai
More
Can anything be done for adults with strabismus (misaligned eyes)?
Yes. Both the variations of adult squint can usually be treated with excellent results. Your doctor will suggest either a surgical or non-surgical treatment, depending on the cause, duration, and severity of the squint.
What causes squint in adults?
The reasons for squint in children and adults are different.
A latent childhood squint may become prominent with eye strain in the later stage of life.
A loss of vision in one eye can result in its outward deviation.
New squint that develops in an adult can be due to disorders of thyroid eye disease, myasthenia gravis, trauma, stroke or tumors.
Sometimes, your doctor cannot determine an identifiable cause for the squint, and these are called idiopathic.
What are the signs and symptoms of squint?
The most noticeable sign of squint, of course, is the misalignment of eyes, which can be noted by the patient, as well as by the observer. Associated symptoms of squint include:
Eye fatigue and tiredness around the eyes
Double vision which can be very annoying, and often leads to intractable headaches
Overlapped or blurred images causing confusion
Difficulty in reading and near work
Loss of depth perception resulting in stumbling and past pointing
What are the benefits of squint surgery in adults?
Many people are of the view that squint surgery in adults is strictly a cosmetic procedure. That is usually not true, and in fact, the operation can result in a significant functional gain. It causes:
Improvement in eye alignment, making the gaze straight
Remove, or at least significantly decrease, diplopia or double vision
Decrease eye fatigue
Provide a definite cosmetic growth, resulting in better social and professional interactions
Who treats squint in adults?
An eye specialist who has had specialized training in strabismus is the most qualified to treat any misalignment of eyes. Usually, ophthalmologists who specialize in the care of children, pediatric ophthalmologists, are also trained in a squint, since the disease is more common in children. That shouldn’t deter you from seeking an appointment with the doctor.
That said, you must evaluate your comfort level with the doctor, his or her bedside manner, credentials, and the hospital/ operation theater facilities before deciding on who can best take care of your eyes.
Utsav Eye Clinic
Dr. Anand Kumar
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
Myth: Cataract is an old age problem
Fact: Most cataracts are senile but can occur at any age. They can also be congenital or caused by steroid intake, injury, diabetes or eye inflammations.
Myth: Cataract can be prevented by medicines, diet, eye exercise or yoga/Cataract can be cured by eye drops, diet or yoga.
Fact: There is no prevention or medical cure for cataracts. The only definitive treatment is cataract surgery. To your surprise, some early cataracts may never progress and may require no treatment if they are not causing any problem in the vision.
Myth: Cataract surgery should be delayed and done only when it matures or ripens.
Fact: The best time to get the surgery done is when you start having early vision problems. There is no point in delaying the surgery too much as the ultrasonic system works faster and is safer on softer cataracts than the hard or mature ones.
Myth: Is it true that cataracts can be removed with lasers without an incision? Or the complete surgery is bladeless and doe with laser only?
Fact: There is no surgery possible without an incision. A cataract is opacity or clouding of the natural lens, which is removed by ultrasonic fragmentation of cataract into tiny pieces by a phaco probe and sucked through a small incision (2.2mm). At present, we are using the Femto laser-bladeless technique of operating cataracts. This technique creates incisions, then the circular opening of the anterior capsule and partial nucleus fragments, which is further followed by routine phacoemulsification with the insertion of the foldable intraocular lens. Hence, laser assists in few steps of phaco surgery but does not completely replace it.
Utsav Eye Clinic
Dr. Anand Kumar
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
Cataract surgery is most often an outpatient procedure, so you will be able to go home the same day your cataract is removed. This means that most of the recovery process will be at home, with some follow-up visits to your ophthalmologist to make sure your eye is healing properly. It is important to closely follow your ophthalmologist’s guidelines for recovery, so you are at less risk of developing complications from the procedure, like inflammation, infection, swelling in the retina, detached retina or lens, pain, and vision loss.
Your ophthalmologist will give you a more detailed schedule of recovery time and expectations, but here are some general recommendations to follow after cataract surgery.
Immediately after surgery:
Once cataract surgery has been completed, and your time in the recovery area has allowed any remaining anesthesia to clear, you can return home. Because your vision will be impacted immediately after surgery, it is not safe to drive yourself home.
.Normal side effects on the first day after surgery include:
- Watery eyes.
- Feeling like you have grit in your eyes.
- Blurry or double vision.
- A red or bloodshot eye.
You may receive medicated eye drops to treat the pain. You should also receive a pair of prescription sunglasses to protect your eyes from the glare of the sun or lights, and it is important to wear these for the length of time recommended by your ophthalmologist. To ensure the safety of your eyes overnight, you may also receive an eye patch or a protective visor to wear to bed so your eye is not hit or poked in your sleep.
Recommendations for Care After Cataract Surgery
In the days and weeks after your surgery, it is recommended that you:
Use prescription eye drops as detailed by your ophthalmologist.
Follow all the recommendations of your ophthalmologist and/or eye surgeon.
Rest and relax for two to three days.
Use your eye shield every night for at least one week.
Wear the eye shield while showering, especially if washing your hair.
Perform normal, low-impact activities like using a computer, reading, or watching TV as normal.
Avoid swimming during recovery for four to eight weeks.
It is important to avoid:
Rubbing your eye.
Getting foreign objects in your eye, like shampoo.
Performing strenuous activities like running or yoga.
Driving before getting the all-clear from your eye doctor.
Flying without your doctor’s knowledge and approval.
You can return to work a few days or weeks after the procedure, depending on what type of job you have.
Utsav Eye Clinic
Dr. Anand Kumar
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
Cataract surgery is a medical procedure that most people will eventually have to go through at some point in life. It’s relatively safe and highly successful eye surgery. However, issues can arise if you have a coexisting retinal disease or other ocular conditions. Dr Anand Kumar, Eye Specialist in Kharghar discusses the common issues that may be co-existing with cataract.
As cataracts develop they make it harder for us to see because the lens becomes opaque – like a dirty window. Once the cloudy cataract is surgically replaced with a clear new lens, we usually see better instantly.
Fortunately, there are things that we can do to prevent this. Here are five things we can do to prevent complications and sudden vision loss after cataract surgery:
1- Take an anti-oxidant, retinal support vitamin formula and take omega 3’s. A green-drink (spirulina, chlorella, algae) will help as well for healing, protecting and nourishing the retina. Liposomal Vitamin C can help if retinal edema becomes present or can be used for prevention.
2- After surgery, it is better to wear UV protective eyewear ANY TIME YOU ARE OUTSIDE during the day… rain or shine! Your eyes are simply not used to the intense UV rays – we can’t just apply sunblock to our retinas. Therefore, we need to use sunglasses to protect our eyes.
4- Wear a hat when you are outside for additional protection from harmful UV rays – especially on rainy days. Protect yourself with sunglasses and a hat for at least 6 weeks after your cataract surgery.
Remember the top three factors that contribute to accelerated vision loss are 1) oxidative stress, 2) inflammation and 3) impaired blood flow. UV radiation accelerates oxidative stress and therefore vision loss in many cases. Taking anti-oxidants and using protection will minimize UV-oxidative stress on the retina and optic nerve.
Discuss about use of anti oxidants with your Eye specialist in Kharghar before starting them.
Dr. Anand Kumar
Utsav Eye Clinic
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
Diwali is the festival of light. Perhaps its most iconic celebration is the colorful and dazzling display of fireworks that lights up the night sky. As beautiful as it looks, fireworks account for thousands of emergency room visits each year during the festival. The majority of injuries that impact eye health occur in bystanders. In fact, the eyes are the second-most common affected area after the hands and fingers. As expected, the leading cause of injuries on Diwali is the lack of appropriate safety measures while lighting fireworks.

Due to serious issues like eye health and safety risks involved, medical experts strongly discourage firework play of any kind. A safer alternative is watching authorized laser and firework displays operated by licensed professionals. But if you still want to use fireworks as part of your celebrations, please ensure you take the following safety precautions at all times:
*Store fireworks in a closed box in a safe location, away from the reach of children
*Avoid sparklers that reach temperatures as high as 1000°C – high enough to melt gold and cause serious injury
*Keep fireworks away from the face, hair, and clothing
*Maintain a distance of an arm’s length while lighting firecrackers, and at least five meters while watching
*Defuse used fireworks properly by soaking them in a bucket of water before disposal
In case of an accident, contact emergency medical services immediately. Do not rub, rinse or apply ointment to the eye. It may make the injury worse or difficult to examine.
By taking these simple precautions for good eye health, you will be able to enjoy fireworks on Diwali without worrying about the safety of your loved ones. Happy celebrations!
Utsav Eye Clinic
Dr. Anand Kumar
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More
If you’re over 50 and your vision has gotten blurry or cloudy, you may have cataracts. It’s a common condition in older adults, and it can be treated by your eye doctor. Dr. Anand Kumar, Cataract Surgeon in Kharghar discusses the common question regarding Cataracts,
What Is a Cataract?
A cataract is a dense, cloudy area that forms in the lens of the eye. A cataract begins when proteins in the eye form clumps that prevent the lens from sending clear images to the retina. The retina works by converting the light that comes through the lens into signals. It sends the signals to the optic nerve, which carries them to the brain.
Symptoms of Cataracts
Common symptoms of cataracts include:
- blurry vision
- trouble seeing at night
- seeing colors as faded
- increased sensitivity to glare
- halos surrounding lights
- double vision in the affected eye
- a need for frequent changes in prescription glasses
What Causes Cataracts?
There are several underlying causes of cataracts. These include:
overproduction of oxidants, which are oxygen molecules that have been chemically altered due to normal daily life
- smoking
- ultraviolet radiation
- the long-term use of steroids and other medications
- certain diseases, such as diabetes
- trauma
- radiation therapy
Types of Cataracts
There are different types of cataracts. They’re classified based on where and how they develop in your eye.
- Nuclear cataracts form in the middle of the lens and cause the nucleus, or the center, to become yellow or brown.
- Cortical cataracts are wedge-shaped and form around the edges of the nucleus.
- Posterior capsular cataracts form faster than the other two types and affect the back of the lens.
- Congenital cataracts, which are present at birth or form during a baby’s first year, are less common than age-related cataracts.
- Secondary cataracts are caused by disease or medications. Diseases that are linked with the development of cataracts include glaucoma and diabetes. The use of the steroid prednisone and other medications can sometimes lead to cataracts.
- Traumatic cataracts develop after an injury to the eye, but it can take several years for this to happen.
- Radiation cataracts can form after a person undergoes radiation treatment for cancer.
Risk Factors of Cataracts
Risk factors associated with cataracts include:
- older age
- heavy alcohol use
- smoking
- obesity
- high blood pressure
- previous eye injuries
- a family history of cataracts
- too much sun exposure
- diabetes
- exposure to radiation from X-rays and cancer treatments
Treatment of Cataracts
Surgery is the only way to get rid of a cataract, but you may not need to get surgery right away. Your doctor might suggest surgery if your cataracts start getting in the way of everyday activities like reading, driving, or watching TV. During cataract surgery, the doctor removes the clouded lens and replaces it with a new, artificial lens (also called an intraocular lens, or IOL).
If you’re unable or uninterested in surgery, your doctor may be able to help you manage your symptoms. They may suggest stronger eyeglasses, magnifying lenses, or sunglasses with an anti-glare coating.
Prevention of Cataracts
To reduce your risk of developing cataracts:
- protect your eyes from UVB rays by wearing sunglasses outside
- have regular eye exams
- stop smoking
- eat fruits and vegetables that contain antioxidants
- maintain a healthy weight
keep diabetes and other medical conditions in check
Dr. Anand Kumar
Utsav Eye Clinic
Utsav Eye Clinic: Eye Clinic in Kharghar | Eye Specialist Doctor
More




